Review Article
Comprehensive Review on Venereal Diseases Transmission: Transmission Routes, Diagnosis, Treatment,
Prognosis, Future Medications, and Recommendations
Abouelhag H. A.
Department of Microbiology and Immunology, National Research
Centre, Dokki, Giza, Egypt, 12622.
Corresponding author: Abouelhag H. A. (Email:
drabouelhag5@gmail.com)
Received: 29-07-2025, Accepted: 16-08-2025. Published
online: 23-08-2025
DOI: https://doi.org/10.33687/ricosbiol.03.08.70
Abstract
Sexually Transmitted Infections
(STIs) are among the most common communicable conditions worldwide, affecting the health and lives of people
globally. The World Health
Organization estimates that over one million new STI infections occur daily among adults aged 15-49. This
comprehensive review aims to provide an in-depth analysis of venereal disease transmission routes, modern
diagnostic methods, available
treatment options, future
prognosis, emerging medications, and preventive recommendations.
This review covers major diseases such as Chlamydia, Gonorrhea, Syphilis, Human Papillomavirus (HPV),
Human Immunodeficiency Virus (HIV), Genital Herpes, and other sexually transmitted infections. It also discusses recent advancements
in molecular diagnostics, antimicrobial resistance, new preventive strategies,
vaccinations, and future therapies. The findings emphasize the importance of early diagnosis,
prompt treatment, and partner management in controlling the spread of these
diseases. Recent data indicate that over 2.4 million cases of Syphilis, Gonorrhea, and Chlamydia were diagnosed
and reported in the United States in 2023, underscoring the continuous need for comprehensive prevention and
treatment strategies.
Keywords: Sexually Transmitted Infections, Venereal Diseases, Transmission Routes, Diagnosis, Treatment, Prevention, Antimicrobial Resistance
Transmission Routes
Sexually Transmitted Infections (STIs) are primarily transmitted from
person to person through unprotected
sexual contact, which includes vaginal, anal, and oral intercourse (CDC, 2021). However,
some STIs can be transmitted through non-sexual means,
making an understanding of transmission mechanisms crucial for prevention and control. Transmission routes can be categorized into several main types:
1.
Direct Sexual Contact
Direct sexual contact
is the most common mode of transmission for most STIs. This occurs
when mucous membranes or bodily fluids (such as semen, vaginal secretions, and blood) from an infected person come
into contact with the mucous membranes or open wounds of an uninfected person.
Diseases transmitted this way include:
Chlamydia and Gonorrhea: These bacteria are primarily transmitted through vaginal, anal, and oral sexual contact. They can affect the genitals,
rectum, and throat (CDC, 2021).
Syphilis: Syphilis is transmitted through
direct contact with syphilitic sores
(chancres) that appear on the genitals, anus, rectum, lips, or mouth (CDC,
2021).
Herpes Simplex
Virus (HSV): Herpes virus is transmitted through direct contact
with herpes sores or the fluids they exude, even in the absence of
visible sores (CDC, 2021).
Human Papillomavirus (HPV): HPV is transmitted through direct
skin-to-skin contact, usually
during sexual activity. It can cause genital warts and certain types of cancer (CDC,
2021).
Human Immunodeficiency
Virus (HIV): HIV is primarily transmitted through unprotected sexual contact (vaginal or
anal) where blood, semen, or vaginal secretions
from an infected person enter the bloodstream of an uninfected person. It can also be transmitted through
oral sexual contact, although this is less common
(CDC, 2021).
2.
Mother-to-Child Transmission (Vertical Transmission)
Some STIs can be transmitted from an infected mother to her child during
pregnancy, childbirth,
or breastfeeding. This type of transmission can cause serious health complications for the infant, including
birth defects, infections, and even death (CDC, 2021). Diseases transmitted vertically include:
Congenital Syphilis: Syphilis bacteria can be transmitted from an infected mother to the fetus during pregnancy, leading to congenital syphilis, which can cause severe
health problems for the infant
(CDC, 2021).
Human Immunodeficiency Virus (HIV): HIV can be transmitted from mother to child
during pregnancy, childbirth, or breastfeeding. However, the risk of transmission can be significantly reduced through antiretroviral therapy for the mother during
pregnancy and childbirth, and by avoiding
breastfeeding (CDC, 2021).
Chlamydia and Gonorrhea: These bacteria
can be transmitted to the infant during
birth, causing eye or lung infections (CDC, 2021).
Genital Herpes:
If the mother
has active herpes
sores during childbirth, the virus can be transmitted to the infant,
causing a serious, potentially life-threatening infection
(CDC, 2021).
3.
Blood Contact
Some STIs can be transmitted through contact with contaminated blood.
This typically occurs through:
Sharing Needles:
Sharing needles or syringes contaminated with blood is a common route of transmission for HIV and
viral hepatitis (B and C) among injecting drug users
(CDC, 2021).
Blood Transfusion and Organ Transplantation: Although now very rare in developed
countries due to rigorous screening of blood and organs, it still represents a potential risk (CDC,
2021).
Needlestick Injuries:
Healthcare
workers can be at risk of bloodborne infections through accidental needlestick injuries (CDC, 2021).
4.
Other (Less Common) Transmission Routes
Direct Non-Sexual Contact: In rare
cases, some STIs can be transmitted through
close skin-to-skin or mucous membrane contact, even without full sexual intercourse. For example, oral herpes can be transmitted through kissing (CDC, 2021).
Contaminated Instruments: Although rare, improperly
sterilized medical or surgical instruments can be a vehicle for the transmission of some STIs (CDC,
2021).
Understanding the various transmission routes highlights the importance
of safe sexual
practices, regular screening, and preventive interventions such as vaccinations (e.g., HPV vaccine) in curbing the spread of STIs (CDC, 2021).
Diagnosis
Early and accurate
diagnosis of Sexually
Transmitted Infections (STIs) is crucial
for preventing serious
health complications and curbing the spread of infection. Diagnostic methods
vary depending on the type of infection and include a wide range of laboratory tests
and clinical examinations (CDC, 2021).
1.
Diseases Characterized by Genital, Anal, or Perianal
Ulcers
These diseases include
Syphilis, Genital Herpes,
Lymphogranuloma Venereum (LGV),
and Granuloma Inguinale (Donovanosis). Diagnosis relies on clinical
observation and laboratory tests:
Syphilis: Syphilis is definitively diagnosed through darkfield microscopy or molecular
tests (PCR) to detect Treponema pallidum directly from lesion exudate
or tissue. Presumptive diagnosis relies on two serologic tests: a
nontreponemal test (VDRL
or RPR) and a treponemal test (TP-PA, EIAs, CIAs, immunoblots, or rapid
treponemal assays). Nontreponemal tests can yield false-positive results and are used to monitor treatment
response, while treponemal tests remain positive for life even after successful treatment (CDC, 2021).
Lymphogranuloma Venereum (LGV): Definitive diagnosis
of LGV requires LGV- specific
molecular testing (e.g., PCR-based genotyping), which is not widely available. Diagnosis is typically based on clinical
suspicion, epidemiological
information, and a Chlamydia trachomatis NAAT at the symptomatic anatomical site, along with the exclusion
of other etiologies (CDC, 2021).
2.
Diseases Characterized by Urethritis and Cervicitis
These include Chlamydia
and Gonorrhea, which are often asymptomatic, especially
in women:
Chlamydia and Gonorrhea: Nucleic Acid Amplification Tests (NAATs) are the preferred
method for diagnosing Chlamydia and Gonorrhea due to their high sensitivity and specificity. Urine samples or swabs from various anatomical sites (cervix, vagina,
urethra, rectum, pharynx)
can be used (CDC, 2021).
Mycoplasma
genitalium: NAATs are the
recommended diagnostic tests for Mycoplasma genitalium. Resistance testing is crucial for guiding treatment
due to increasing antimicrobial resistance (CDC, 2021).
3.
Diseases Characterized by Vulvovaginal Itching, Burning, Irritation, Odor, or Discharge
These include Bacterial Vaginosis
(BV), Vulvovaginal Candidiasis (VVC), and Trichomoniasis:
Bacterial Vaginosis (BV): Diagnosis relies on microscopic examination
of wet mount showing clue cells, an elevated pH (>4.5), and a KOH
test yielding an amine odor.
Clinical laboratory tests
can also be used (CDC, 2021).
Vulvovaginal
Candidiasis (VVC): Diagnosis relies on clinical
indicators such as vulvar itching and pain, and microscopic examination showing budding yeasts or pseudohyphae. VVC is associated
with a normal vaginal pH (<4.5). Yeast culture is the gold standard
for diagnosis (CDC, 2021).
4.
Other Diseases
Human Immunodeficiency Virus (HIV): HIV infection
is diagnosed by HIV 1/2 Ag/Ab combination immunoassays. The CDC recommends that HIV testing
begin with a laboratory-based
HIV-1/HIV-2 Ag/Ab combination assay, followed by a laboratory-based assay with a supplemental HIV-1/HIV-2 antibody differentiation assay if repeatedly reactive (CDC, 2021).
Viral Hepatitis
(B and C): Viral Hepatitis (B and C) is diagnosed
through blood tests
that detect antigens,
antibodies, and viral nucleic acid (CDC,
2021).
Human Papillomavirus (HPV): HPV is typically diagnosed through
Pap tests to detect cellular
changes, and HPV DNA tests to detect
high-risk viral types (CDC,
2021).
Regular screening, especially for at-risk individuals, is vital for early
diagnosis and effective intervention.
Accurate diagnosis also guides appropriate treatment and reduces the risk
of transmission (CDC, 2021).
Treatment
The treatment of Sexually Transmitted Infections (STIs) depends on the
type of infection, whether bacterial,
viral, fungal, or parasitic. The goal of treatment is to eliminate the pathogen, alleviate symptoms, prevent
complications, and stop the transmission of infection to others. It is essential
to adhere to the full and recommended doses of
medications, even if symptoms disappear, to ensure complete cure and prevent
the development of antimicrobial resistance (CDC, 2021).
1.
Curable Bacterial Infections
Bacterial infections are treated with antibiotics and are curable if
diagnosed and treated early:
Syphilis: Penicillin G is the preferred drug for all stages of syphilis, administered parenterally. The dosage and duration of treatment depend on
the stage of the disease and clinical
manifestations. Patients should be informed about the potential Jarisch-Herxheimer reaction, an acute febrile reaction that can occur within
24 hours of syphilis therapy
(CDC, 2021).
Chlamydia: Doxycycline 100 mg orally
twice daily for 7 days is the recommended treatment. Azithromycin 1 gram orally as
a single dose can be used as an alternative, especially during pregnancy (CDC, 2021).
Gonorrhea: Gonorrhea treatment has become complicated due to the ability of Neisseria gonorrhoeae to develop resistance
to available antibiotics. The 2021 CDC guidelines recommend ceftriaxone 500 mg intramuscularly as a single
dose. Dual therapy with azithromycin or doxycycline, previously recommended, is no longer advised
due to concerns about azithromycin resistance (CDC,
2021).
Mycoplasma
genitalium: Resistance-guided therapy is emphasized due to increasing
antimicrobial resistance. A two-stage approach is recommended: an initial
dose of doxycycline to reduce the microbial
load, followed by either high-
dose azithromycin (for macrolide-sensitive infections) or moxifloxacin
(for macrolide-resistant infections).
If resistance testing is not available, doxycycline followed by moxifloxacin is recommended (CDC, 2021).
Bacterial Vaginosis (BV): Metronidazole 500 mg orally twice daily for 7 days, or metronidazole gel 0.75% intravaginally,
or clindamycin cream 2% intravaginally are
recommended. Women should be advised to abstain from sexual activity or consistently use condoms during
the treatment period
(CDC, 2021).
Pelvic Inflammatory Disease
(PID): Empiric treatment for PID should be initiated in sexually active young women
and other women at risk for STIs if they experience
pelvic or lower abdominal pain. Recommended regimens include a combination of intravenous or intramuscular antibiotics, such as ceftriaxone with doxycycline and metronidazole (CDC, 2021).
Epididymitis: Treatment depends
on the likely cause. If caused by Chlamydia or Gonorrhea, ceftriaxone 500 mg IM as a single dose plus doxycycline 100 mg orally
twice daily for 10 days is recommended. If caused by enteric organisms, levofloxacin is recommended (CDC, 2021).
2.
Chronic Viral Infections
There is no cure for most viral
STIs, but symptoms
can be managed and recurrence reduced:
Human Immunodeficiency
Virus (HIV): Antiretroviral therapy (ART) should be initiated
as soon as possible for all persons
with HIV infection, regardless of CD4+
T-cell count. ART significantly reduces transmission, improves laboratory markers, decreases acute disease severity,
lowers viral setpoint, reduces viral reservoir size, decreases viral mutation rate, and preserves
immune function (CDC, 2021).
Genital Herpes: Antiviral medications such as acyclovir, valacyclovir, and famciclovir are used to manage herpes outbreaks and reduce recurrence. These drugs do not eliminate the virus from the body but help control symptoms
(CDC, 2021).
Human Papillomavirus
(HPV): There is no cure for HPV itself, but
clinical manifestations such as
genital warts can be treated. Treatment options include surgical removal of warts, cryotherapy, laser therapy, or topical medications. HPV
vaccines are an effective means of preventing infection and associated cancers (CDC, 2021).
Viral Hepatitis (B and C): Effective treatments are available for Hepatitis C that can lead to complete cure in most cases.
For chronic Hepatitis B, antiviral medications can control the virus and prevent liver damage (CDC, 2021).
3.
Fungal and Parasitic Infections
Vulvovaginal
Candidiasis (VVC): VVC is treated with short-course topical
formulations (single dose or 1-3 day
regimens) or a single oral dose of fluconazole.
These treatments are effective in relieving symptoms and eradicating the infection (CDC, 2021).
Trichomoniasis: Trichomoniasis is treated with oral metronidazole or tinidazole. It is important to treat sexual partners simultaneously to prevent reinfection (CDC, 2021).
Adherence to treatment, partner management, and regular follow-up are
crucial for successful treatment and reducing the spread of STIs (CDC, 2021).
Prognosis
The prognosis of Sexually Transmitted Infections (STIs) largely
depends on the type of infection, the stage of diagnosis, adherence to treatment, and the
presence of any complications. While many STIs are completely curable if diagnosed and
treated early, others can cause chronic
or even life-threatening health problems if left untreated (CDC, 2021).
1.
Curable Bacterial Infections
Chlamydia and Gonorrhea: If diagnosed and treated early with appropriate antibiotics, the prognosis is excellent, and complete recovery
usually occurs without complications.
However, if left untreated, they can lead to serious complications such as Pelvic Inflammatory Disease (PID) in women, which can cause infertility, ectopic pregnancy,
and chronic pelvic pain. In men, they can cause epididymitis, which may affect fertility (CDC, 2021).
Syphilis: Syphilis can be effectively treated with penicillin, especially in the early stages
(primary, secondary, and early latent syphilis). The prognosis is very good with proper treatment. However,
if the disease progresses to late stages (late
latent syphilis, tertiary
syphilis, neurosyphilis), it can cause irreversible damage
to vital organs such as the heart, brain, and nervous system, leading to
chronic health problems, disability, and in some cases,
death (CDC, 2021).
Bacterial Vaginosis (BV) and Trichomoniasis: These infections are curable with antibiotics. The prognosis is good with treatment.
However, they can increase the risk
of acquiring other STIs and cause pregnancy complications if left untreated
(CDC, 2021).
2.
Chronic Viral Infections
Human Immunodeficiency Virus (HIV): There is currently no cure for HIV, but with effective
Antiretroviral Therapy (ART),
people living with HIV can lead long and healthy
lives. ART reduces
the viral load to undetectable levels, preventing the progression to AIDS and significantly reducing
the risk of HIV transmission. However, treatment requires
lifelong adherence (CDC, 2021).
Genital Herpes:
There is no cure for genital herpes,
and the virus
remains in the body
for life. However, antiviral medications can reduce the frequency and severity
of outbreaks. The prognosis is good in terms of symptom management, but the infection
can cause psychological and social distress
(CDC, 2021).
Human Papillomavirus
(HPV): Most HPV infections clear on their own
without intervention. However,
some high-risk HPV types can lead to the development of cervical, anal, oral, and throat cancers,
among others. The prognosis depends
on early detection and
treatment of cellular changes. HPV vaccines offer excellent protection against infection and associated cancers
(CDC, 2021).
Viral Hepatitis B and C: Hepatitis B can become chronic and lead to cirrhosis and liver cancer. Antiviral treatments are
available that can control the virus. Hepatitis C, in contrast,
can be effectively cured in most cases using direct-acting antiviral medications, leading to complete recovery and
preventing long-term complications (CDC, 2021).
3.
Long-Term Complications
If left untreated, STIs can lead to a wide range of long-term complications, including:
Infertility: Untreated Chlamydia
and Gonorrhea can cause damage to the fallopian tubes in women, leading to infertility or ectopic pregnancy
(CDC, 2021).
Chronic Pelvic
Pain: Can be a result of recurrent or untreated Pelvic
Inflammatory Disease (CDC, 2021).
Increased Risk of HIV Acquisition: Other STIs, especially those causing ulcers,
can
increase the risk of acquiring
and transmitting HIV (CDC,
2021).
Cancer: Certain HPV types are associated with cervical, anal,
oral, and throat
cancers. Hepatitis B and C are linked
to liver cancer
(CDC, 2021).
Infant Health
Problems: Mother-to-child transmission of STIs can lead to serious health problems for the infant,
including blindness, deafness, brain damage, and death (CDC,
2021).
Overall, the prognosis emphasizes the importance of regular screening, early diagnosis, prompt treatment, and partner management to reduce the negative health
consequences of STIs
(CDC, 2021).
Future Medications and Therapeutic Innovations
The field of Sexually Transmitted Infections (STIs) treatment is
undergoing continuous development, driven by the need to overcome antimicrobial resistance,
improve treatment efficacy,
and provide more convenient options
for patients. Current
research focuses on developing new drugs,
preventive and therapeutic vaccines, and innovative strategies for pre-exposure and post-exposure prophylaxis (CDC, 2021).
1.
New Antibiotics to Combat Resistance
Antimicrobial resistance poses a significant challenge in the treatment of
bacterial STIs, especially Gonorrhea.
Efforts are focused on developing new classes of antibiotics
or repurposing existing
drugs:
Gonorrhea
Treatments: Given the increasing
resistance of Neisseria gonorrhoeae to available antibiotics, there is an urgent
need for new drugs. Research is underway on compounds such as Zoliflodacin and Cefiderocol, which
have shown promising results in clinical trials against resistant
Gonorrhea strains (CDC, 2021).
Mycoplasma genitalium Treatments: With increasing resistance of Mycoplasma genitalium to macrolides and fluoroquinolones, alternative drugs or new
combination therapies are being explored.
Research focuses on understanding resistance mechanisms to develop
targeted treatments (CDC, 2021).
2.
Preventive and Therapeutic Vaccines
Vaccines are powerful tools for preventing infectious diseases, and there
are intensive efforts to develop vaccines
against STIs for which no vaccines are currently available:
Gonorrhea Vaccine: Several vaccine candidates against Gonorrhea are under development, targeting
bacterial surface proteins
to prevent infection
or reduce its severity. Some vaccines used against
meningococcal meningitis (which resembles
Neisseria gonorrhoeae) show some cross-protection against Gonorrhea (CDC, 2021).
Chlamydia Vaccine:
No vaccine is currently available for Chlamydia, but research is ongoing to develop vaccines
targeting Chlamydia trachomatis proteins to prevent
infection or reduce
complications (CDC, 2021).
Genital Herpes Vaccine: Although vaccines
against Herpes Simplex Virus (HSV) are in early stages of development, no commercially available
effective vaccine is currently available to prevent genital
herpes (CDC, 2021).
HIV Vaccine: Despite significant progress
in antiretroviral therapy,
developing an effective HIV vaccine remains
a top priority. Research focuses
on inducing broad immune responses that can neutralize different viral strains
(CDC, 2021).
3.
Pre-Exposure Prophylaxis (PrEP) and Post-Exposure Prophylaxis (PEP)
Pre-Exposure Prophylaxis (PrEP)
and Post-Exposure Prophylaxis (PEP) strategies are highly effective in preventing HIV transmission, and similar applications
are being explored for other STIs:
STI PrEP: The use of
antibiotics (such as doxycycline) as pre-exposure prophylaxis (Doxy-PEP) is being investigated to reduce the risk of Chlamydia, Gonorrhea, and Syphilis in high-risk
groups. Studies have shown promising results in reducing the incidence of these diseases
(CDC, 2021).
STI PEP: Similar
to HIV PEP, the use of antibiotics after sexual exposure is being evaluated
to reduce the risk of bacterial STIs (CDC,
2021).
4.
Gene Therapy and Immunotherapies
Gene therapy and immunotherapies are promising research areas for chronic
STIs such as HIV and
Herpes:
![]() Gene Therapy for HIV: Some research
aims to modify a patient's
immune cells to make
them resistant to HIV infection, or to enable the body to produce neutralizing antibodies (CDC, 2021).
Gene Therapy for HIV: Some research
aims to modify a patient's
immune cells to make
them resistant to HIV infection, or to enable the body to produce neutralizing antibodies (CDC, 2021).
Immunotherapies for Herpes: Focus on enhancing the immune system's
response to control
the virus and reduce the frequency of outbreaks (CDC, 2021).
5.
Point-of-Care Testing
(POCT)
Developing rapid point-of-care tests is crucial for improving early
detection and prompt treatment, thereby reducing transmission. Research focuses on developing rapid and accurate tests
that can be performed outside
the laboratory (CDC, 2021).
These developments demonstrate a global commitment to combating STIs and offer hope for a future where these diseases
are more preventable and treatable (CDC, 2021).
Recommendations
Controlling Sexually Transmitted Infections (STIs) requires a
comprehensive and multifaceted approach that combines prevention, early diagnosis, effective
treatment, partner
management, and health education. Based on available information and ongoing challenges, the following recommendations can be made:
1.
Enhance Health Education and Awareness
Comprehensive Education
Programs: Implement comprehensive health education programs on STIs in schools and
communities, focusing on transmission routes,
the importance of safe sexual
practices, early diagnosis, and treatment. These
programs should be age-appropriate and culturally sensitive (CDC, 2021).
Public Awareness Campaigns: Launch public awareness
campaigns targeting high-risk populations, including youth and marginalized groups, to increase
awareness
of risks, encourage
regular screening, and reduce the stigma associated with
STIs (CDC, 2021).
2.
Expand Screening
and Diagnosis
Routine Screening: Integrate routine STI screening into primary healthcare, especially for sexually active
individuals and high-risk groups. Screening should
be accessible, convenient, and confidential (CDC, 2021).
Point-of-Care Tests (POCT): Invest in the development and deployment of rapid and accurate point-of-care tests for
STIs, enabling immediate diagnosis and treatment at the same visit, thereby reducing loss to follow-up
and interrupting the chain
of transmission (CDC, 2021).
Partner Screening: Encourage
the screening and treatment of sexual partners
of individuals diagnosed with STIs to prevent
reinfection and curb their spread (CDC,
2021).
3.
Improve Access to Treatment
and Care
Prompt Treatment: Ensure immediate access to appropriate and effective treatment for individuals diagnosed with STIs. Medications should be available and affordable (CDC, 2021).
Antimicrobial Resistance Management: Develop and implement
strategies to monitor
antimicrobial resistance patterns of STIs and guide treatment based on local resistance patterns. Invest in
research and development of new drugs to combat increasing resistance (CDC, 2021).
Comprehensive Care: Provide comprehensive care for individuals with STIs, including counseling, psychological support,
and reproductive health services (CDC,
2021).
4.
Strengthen Prevention Strategies
Condoms: Promote the consistent and correct use of condoms
as an effective means of preventing most STIs (CDC, 2021).
Vaccinations:
Expand vaccination programs against Human Papillomavirus (HPV) and Hepatitis B, and invest
in the development of new vaccines against
other STIs (CDC, 2021).
Pre-Exposure Prophylaxis (PrEP) and
Post-Exposure Prophylaxis (PEP): Expand the use of PrEP and PEP for HIV, and explore similar applications for bacterial STIs, such as Doxy-PEP, for high-risk groups
(CDC, 2021).
Male Circumcision: Promote male circumcision in regions with high rates of HIV and other STIs, as studies have shown it reduces the risk of acquiring certain
STIs (CDC,
2021).
5.
Research and Development
Investment in Research: Increase investment in research and development for new drugs,
vaccines, innovative diagnostic methods, and prevention strategies. Research
should focus on a better understanding of the epidemiology, biology, and immunology of STIs (CDC, 2021).
International
Collaboration: Foster international collaboration and the exchange of information and expertise
among countries and organizations to combat STIs on a global scale (CDC,
2021).
By implementing these recommendations, communities can make significant
progress in
reducing the burden of STIs and improving sexual and reproductive health worldwide
(CDC, 2021).
Tables and Figures
Table 1: Key STI Statistics (2020-2023)
|
Source |
Statistic Type |
Value |
Notes |
|
CDC (2023) |
Total Syphilis, Gonorrhea, and Chlamydia Cases |
> 2.4 million |
Diagnosed and reported
in the United States |
|
CDC (2023) |
Syphilis Cases |
> 209,000 |
In the United States |
|
CDC (2023) |
Gonorrhea Cases |
> 600,000 |
In the United States |
|
CDC (2023) |
Chlamydia Cases |
> 1.6 million |
In the United States |
|
CDC (2023) |
Congenital Syphilis Cases |
3,882 |
In the United States,
including 279 stillbirths/infant deaths |
|
WHO (2020) |
New infections of Chlamydia, Gonorrhea, Syphilis, or Trichomoniasis |
374 million |
Among adults aged 15-49 globally |
|
WHO (2020) |
New cases daily |
> 1 million |
Among adults aged 15-49 globally |
|
WHO (2022) |
New Syphilis infections |
8 million |
Among adults aged 15-49 globally |
|
WHO (2022) |
Congenital Syphilis Cases |
700,000 |
Globally |
|
CDC (2012- 2016) |
HPV-associated cancers |
34,800 |
New cases
annually in the United States |
|
CDC (pre- vaccine) |
HPV-associated genital warts |
355,000 |
New cases
annually in the United States |
Figure 1: Sexually Transmitted Infection
Transmission Routes

Description: This figure illustrates the main transmission routes of sexually
transmitted infections, including unprotected sexual contact,
blood transfusion, needle reuse, and mother-to-child transmission during pregnancy.
Figure 2: Sexually
Transmitted Infection Diagnosis
Methods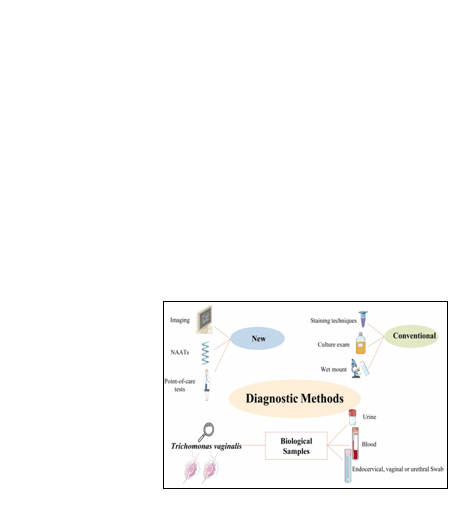


Description: This figure illustrates various diagnostic techniques used to detect sexually
transmitted infections, ranging
from wet mount microscopy to Nucleic Acid
Amplification Tests (NAATs).
Figure 3: Sexually Transmitted Infection Treatment Guidelines

Description: This figure represents the Sexually Transmitted Infection Treatment Guidelines issued by
the Centers for Disease Control and Prevention (CDC), providing updated
recommendations for healthcare professionals.
References
[1]
Centers for Disease
Control and Prevention. (2021). Sexually Transmitted Infections Treatment Guidelines,
2021.
U.S. Department of Health and Human Services. https://www.cdc.gov/std/treatment-guidelines/STI-Guidelines-2021.pdf
[2]
World Health Organization. (n.d.). Global and regional STI estimates. Retrieved
from https://www.who.int/data/gho/data/themes/topics/global-and-regional-sti-estimates
[3]
Centers for Disease Control and Prevention. (2023). National Overview of STIs in 2023. Retrieved from https://www.cdc.gov/sti-statistics/annual/summary.html